

In December 2025, The Michael J. Fox Foundation (MJFF) hosted a panel discussion on stress and Parkinson’s disease (PD). The panel tackled how stress affects Parkinson’s symptoms and why stress happens. They explained the difference between acute stress (normal and temporary) and chronic stress (which causes real problems), and walked through the brain mechanisms that make symptoms worse when someone is stressed. Read our notes.
The panelists included Becca Miller (clinical psychologist at Yale, diagnosed with PD in 2013), Dr. Rick Helmich (neurologist at Radboud University in the Netherlands), Dr. Amie Hiller (movement disorder specialist at VA Portland), and Jim McNasby (General Counsel at The Michael J. Fox Foundation, diagnosed with PD in 2000), who moderated the discussion.
What made this session valuable was the combination of neuroscience and lived experience. The panelists didn’t just explain the science, they shared their own stories about stress making symptoms worse, the self-consciousness that compounds the problem, and practical strategies for managing it all. They also answered a question that many people have: does stress actually cause Parkinson’s? The answer surprised me.
Watch the full webinar on The MJFF YouTube channel:
Webinar: “Stress and Parkinson’s: Strategies to Manage the Strain” December 2025
Webinar slides (PDF): Stress and Parkinson’s: Strategies to Manage the Strain
Related resources from the Stanford Parkinson’s website:
Related resource from the American Parkinson Disease Association:
Resource mentioned in the webinar:
- Hidden Disabilities Sunflower – International symbol lanyard/badge for airport assistance
Audience questions were addressed throughout the discussion. Now, on to my detailed notes. – Kevin
Stress and Parkinson’s – Strategies to Manage the Strain
Panelists

- Becca Miller (licensed clinical psychologist and associate professor, Department of Psychiatry, Yale School of Medicine; diagnosed with PD in 2013; member of Michael J. Fox Foundation’s Patients Council)

- Dr. Rick Helmich (neurologist, Radboud University Medical Center, Netherlands; principal investigator at the Donders Center leading the systems neurology group; research focus on stress and Parkinson’s)

- Dr. Amie Hiller (movement disorder specialist and director of the Northwest Parkinson’s Disease Research, Education and Clinical Centers at VA Portland Health Care System; associate professor of neurology, Oregon Health and Science University)

- Jim McNasby (General Counsel, The Michael J. Fox Foundation; diagnosed with PD in 2000; moderator)
Webinar Date: December 18, 2025
Host: The Michael J. Fox Foundation (MJFF)
Summary by: Kevin Boyd, Stanford Parkinson’s Community Outreach
The Stress Cycle: What Happens in Your Body
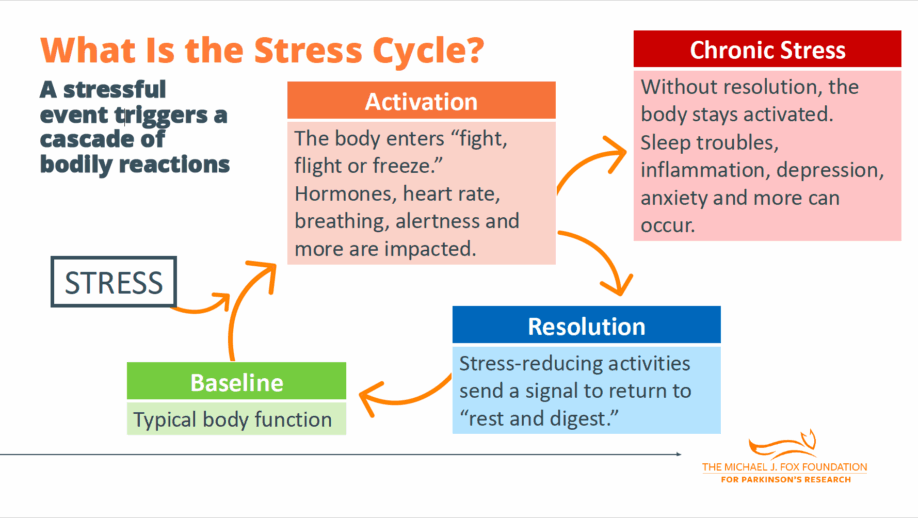
Dr. Hiller explained that stress is complicated, with many effects. You can have an increase in heart rate and cortisol levels. In Parkinson’s, you may have worsening of some symptoms. There are a number of things that happen during a stress response.
When asked about the difference between “good stress” (like a wedding, travel, or birth of a family member) and “bad stress,” Dr. Hiller said all stress in the acute phase has similar effects, which is not necessarily bad: it’s expected and normal. We should get stressed with things.
But the problem is if you stay at that high stress level and can’t come back down. Chronic stress is the real issue. The normal up and down isn’t so bad. That could happen with good stress, good activities, good things happening, but it could also happen with bad things.
“And I think it’s important to keep in mind that any stress is stress even when it’s a good thing. So, you know, to just think about how you manage that,” Dr. Hiller said.
Jim McNasby added: “I also think about having no stress is not necessarily a good thing. You want to have a little stress which goes along with good things happening, right? You want there to be good things in your life that may cause a little stress, but then you can recover from it fairly easily, whereas chronic stress can cause more problems.”
How the Stress Cycle Works
Dr. Helmich walked through the physiological stress cycle:
When people are stressed, the first thing that happens is a surge of noradrenaline in the brain, and that acts really fast: within seconds. It pushes your heart rate up, makes your pupils go wider, and it also has effects on brain areas that are important for some symptoms of Parkinson’s disease. For example, the thalamus, which plays a role in tremor.
Those are the acute effects. Then after a few minutes, maybe 10 to 15 minutes, cortisol starts to rise and has an effect for about half an hour or an hour. But after that, if the stress is gone, that cortisol is back to normal.
In people who experience chronic stress, that cortisol doesn’t go down again. It stays up and it might have effects on the brain as well that are not good.
Stress, Depression, and Anxiety: How They Relate

Dr. Helmich addressed the relationship between chronic stress and mental health conditions like depression and anxiety.
There are some of the same symptoms: stress may affect your sleep, depression affects sleep, anxiety can affect sleep. But they’re not necessarily the same.
Depression is more associated with sadness and hopelessness. Anxiety is more agitation, whereas stress can feel like you’re kind of more activated. They all may benefit from something like psychotherapy, but they have different underlying mechanisms.
Depression and anxiety can also often fall together. So there’s a lot of overlap, but there are certain specific differences that a mental health professional or someone else can really help you tease out.
Personal Experiences With Stress and PD
Becca Miller shared her own experience with how stress manifests with her Parkinson’s symptoms:
“Yeah, for sure. I mean, I think it goes one of either two ways. It can cause me to have more dyskinesia: it sort of activates that end, or it can cause my medications not to work as well. So it kind of goes both ways.”
She doesn’t experience tremor, but she’s heard from a lot of people how stress really activates tremor in a lot of ways. “And then there’s this kind of cycle of feeling more embarrassed, you know, being more tremulous, and then it can be a sort of bad cycle in that way.”
Jim McNasby shared his own perspective: “I think of it in my own experience as kind of a vicious cycle because the stress begets worse symptoms, begets more stress, and you just keep going down. And I find myself becoming clumsy with my speaking, with my gestures, with my tremor, which is really well controlled by DBS that I had six years ago. But you know, when I’m about to do something like talk to a lot of people on the webinar, I find myself halting and my symptoms become more. So I try to be aware of that and not worry about it because the self-consciousness can really kick in, and then that’s the worst.”
Symptoms That Worsen With Stress
Dr. Hiller described what she sees in her patients when they’re stressed:
“So some of the things you both already mentioned: tremor is one that I think for a lot of people, I sometimes call it people’s stress-o-meter. You know, as soon as their tremor really kicks up, it’s like, ‘Oh, okay, I’m stressed,’ and maybe they don’t want to think they are, but that tremor kind of keeps them in check of knowing when they are.”
Dyskinesia certainly gets worse. Freezing of gait is another one where people kind of have their feet get stuck to the floor and have trouble with walking. “Those are kind of the three I would say we think of most commonly as getting worse with stress.”
Why Medications Seem Less Effective When Stressed
An audience member asked why medications seem less effective when stressed.
Dr. Hiller explained it’s probably a combination. One, if the symptoms are worse, it’s going to be harder to manage the symptoms. Also, your metabolism may be going faster when you’re stressed and kind of working through those meds, so they may not last as long.
Jim McNasby added: “Yeah, it often feels like I burn through my dopamine faster when I’m stressed, and then more off periods come.”
The Neuroscience: Why Stress Causes These Effects
Dr. Helmich explained why stress causes these effects in people with Parkinson’s:
“So stress has multiple effects on the brain.” The hyperkinetic movements like tremor or dyskinesia are the clearest or most visible effects of stress on people with Parkinson’s. He thinks this is caused by the effects of noradrenaline, which acts on motor regions in the brain.
In healthy people and everyone, this also has a role: if you’re in stress, you need to act fast, you need to either run away or fight or whatever. So noradrenaline has an effect of activating those motor regions. In people with Parkinson’s disease, the effect is that things like tremor and dyskinesia go up.
But there’s another mechanism: “People with Parkinson’s disease often experience that the things that should normally go automatically don’t go automatically anymore. So you have to more consciously think about things that you are doing, and that requires extra effort of several brain regions. That is something that we call compensation: the healthy part of the brain compensates for those difficulties with doing automatic things.”
What stress does is basically wipe away these compensatory mechanisms. “And that is why a lot of other problems that patients experience become worse when they are stressed.”
Does Stress Cause Parkinson’s?
An audience question addressed whether stress actually causes Parkinson’s, as many people are diagnosed at a particularly stressful point in their life.
Dr. Helmich responded that many people indeed are diagnosed after a very stressful event. He had one woman who developed her first tremor the day after her husband experienced a severe heart attack, and another patient who developed or noticed her first tremor while she was at her mother’s funeral. Others experience their first symptoms like tremor when they recover from anesthesia after surgery.
“Many people tend to think that this event indeed caused Parkinson’s. I don’t think that is the case,” Dr. Helmich said. “And the reason is that Parkinson’s disease already affects the brain 5 to 10 years before the very first symptoms emerge. So there’s a very long period in which Parkinson’s disease is already present in the brain, but it doesn’t cause symptoms, and that is because these compensatory mechanisms are in place in the brain to prevent these symptoms. And when a very stressful event occurs, those compensatory mechanisms are transiently wiped away and Parkinson’s disease is unmasked. So it shows itself, but that doesn’t mean that the stress caused it. It just means that it became visible at that time.”
Beyond Motor Symptoms: Stress and Daily Life
Becca Miller talked about how stress affects her non-motor symptoms. Sleep is definitely affected, which is not uncommon for anyone when they’re stressed to have more sleep problems, but certainly with Parkinson’s, she already has trouble staying asleep. So it definitely affects that.
Executive functioning is also affected: being able to plan and carry out things. “When I’m stressed, it’s much harder for me to do things like that,” she said.
Jim McNasby reflected on his own experience: “I was a very young and ambitious lawyer, and I got this heavy diagnosis when I was 31, and my stress level was off the charts. And it took me a while to realize that my symptoms were in part being worsened by the combination of stress and Parkinson’s. And it really led me to be afraid and led me to think my prognosis or my diagnosis path was going to be much worse than it’s actually been. So I’ve made some changes over time to reduce that, but that concentration of the two things together is very consequential and very something that can be difficult to deal with.”
PTSD and Parkinson’s Risk
An audience member asked how PTSD relates to Parkinson’s and whether a history of PTSD has an impact on developing Parkinson’s.
Dr. Hiller said researchers at the VA have been looking at this, and it does seem like it’s an increased risk factor for developing Parkinson’s disease. This was looking at a big data set. There are always questions on that type of data: is it fully good data? Also, are people who experience PTSD more likely to have had head traumas? There are other things that go along with that. But it does look like there might be a suggestion that PTSD is a risk factor for developing Parkinson’s, but it’s hard to say that for sure.
Diet and the Gut-Brain Connection
Dr. Helmich discussed the relationship between the gut and the brain. There are a lot of neurons in the gut, so the brain and the gut communicate. What studies there are seem to show that a Mediterranean diet (lots of vegetables, lots of fibers) is good for improving gut health, and that might also have an effect on stress and motor symptoms.
Practical Tips for Managing Stress
Traveling With Parkinson’s
Several practical tips emerged for reducing travel stress. Try to have an aisle seat, it’s easier to maneuver. Don’t carry too many things; check a bag instead of carry-on. Build in extra time and start packing early so it’s not stressful. Don’t build in a really tight schedule; leave space to recover.
Becca Miller mentioned the Hidden Disabilities Sunflower, a lanyard and badge you can get online. This is an international symbol of a hidden disability that can help airport staff recognize you may need extra time or assistance.
Finding Community Support
Becca Miller talked about finding community support. There are many different ways depending on what works for you: Facebook groups, local area support groups, your local area agency on aging, and online communities where you can connect with people all over the country and world, in different time zones.
Jim McNasby encouraged everyone to use the buddy network, offered by the foundation.
For Caregivers: You Can’t Pour From an Empty Cup
The final question asked each panelist for wisdom for caregivers.
Dr. Hiller: “Becca said something about thinking about the things that cause you stress and is there a way to get rid of those? I think for caregivers that’s really huge. Are there people that you can hire to do certain things? Are you living in a very large house with stairs that makes it tough for your partner to get up and down? Are there ways you can simplify life and make things easier on yourself? And I think to not feel guilty about those changes, but really take advantage of those changes so that you can kind of get some things off your plate, because oftentimes it overflows.”
Becca Miller: “Yeah, I think you can’t pour from an empty cup is a phrase I saw recently, which is so important. I think, you know, oftentimes it can feel like the focus is all on the person with PD, but the caregiver needs to have time for themselves and to really focus on their own mental health and wellness, and just to take that time is so important.”
Dr. Helmich: “Yeah, I think it’s really important that the system, the caregiver and the patient, are both in balance. So I guess my main advice would be to speak to each other about what causes stress, not only in the person living with Parkinson’s but also in the caregiver. We sometimes have shared sessions where a psychotherapist, for example, speaks to both the caregiver and the patient. So that might sometimes work. And shame is often a big thing that creates this vicious circle. So sometimes it can also really help to explain to the people around you, or even in a restaurant, why you’re having tremor and try to break that cycle of shame and stress and more symptoms, and ultimately preventing you from doing stuff.”
Jim McNasby concluded: “Thank you all for those answers. And then I would just conclude by saying to all the caregivers listening, thank you for doing everything that you do, because all of us who have this scourge depend on you for everything. Thank you for being part of our community and for joining us today.”