

Dr. Ray Dorsey, director of the Center for Brain and Environment at the Atria Health and Research Institute, visited the Bay Area in January 2026 as part of his national book tour for “The Parkinson’s Plan,” (pdplan.org), co-authored with Dr. Michael Okun. Stanford’s APDA Information & Referral Center hosted Dr. Dorsey at two local venues. During the two talks, Dr. Dorsey presented the hypothesis: Parkinson’s disease (PD) is not a natural consequence of aging but an unnatural one, driven primarily by environmental chemical exposures, not by genetics.
The talks focused on three environmental exposures:
- trichloroethylene (TCE), a degreasing and dry cleaning chemical that contaminates up to 30% of U.S. groundwater and is present at 15 superfund sites in Silicon Valley alone. Dr. Dorsey detailed how TCE exposure at Marine Corps Base Camp Lejeune resulted in a 70% increased risk of PD among Marines who served there, and how female dry cleaning workers in Denmark had a 1,500% increased risk of developing the disease.
- paraquat, a weed killer banned in 50 countries including China but still widely used in American agriculture; and
- air pollution, which costs humans an average of three years of life and can penetrate the olfactory nerve to bring toxic metals into the brain.
Dr. Dorsey outlined “The Parkinson’s 25,” a set of practical steps people can take to reduce their risk of developing PD or slow its progression if already diagnosed. These include filtering water, washing produce, using air purifiers, exercising regularly, following a Mediterranean diet, and ensuring quality sleep. He emphasized that it’s never too late to take action, citing studies showing that stopping exposure to harmful chemicals can reduce disease risk, just as stopping smoking reduces lung cancer risk.
The conversations concluded with a passionate call to action. Dr. Dorsey said he sees people with PD as robbery victims: robbed of their independence, incomes, professions, and future plans. He believes society is “asleep” to what the evidence already shows: that PD is largely preventable through both individual actions and collective policy changes, including banning harmful chemicals and cleaning up contaminated sites.
Dr. Dorsey referred to many research studies. We’ve provided links to those published papers at the bottom of our notes. And he mentioned tasks like locating Superfund sites near you and washing produce. We’ve provided relevant links at the bottom of our notes.
The Stanford APDA I&R Center Coordinator Robin Riddle interviewed Dr. Dorsey in conversations that welcomed audience questions. The two discussions, including questions and answers, are aggregated below. Now, on to my detailed notes. – Kevin
A New Path to Parkinson’s Prevention and Treatment

Speaker: Ray Dorsey, MD: director, Center for Brain and Environment at the Atria Health and Research Institute (atria.org), NYC, and movement disorder specialist, University of Rochester
Seminar Date: January 28, 2026. Two locations in the San Francisco Bay Area.

Host: Stanford APDA Information & Referral Center (parkinsons.stanford.edu). Moderated by Robin Riddle, Stanford APDA I&R Center.
Summary by: Kevin Boyd, Stanford Parkinson’s Community Outreach
The Rise of Parkinson’s Disease
When Dr. James Parkinson described the condition in 1817 at the height of the Industrial Revolution amidst London’s fog, he documented something he believed was new. He described six individuals, all likely men, all over 50 years old with symptoms consistent with what we now call Parkinson’s disease. Two hundred years later, an estimated six million people worldwide had Parkinson’s disease (PD). As of 2021, just four years later, approximately 11.77 million people worldwide were living with Parkinson’s disease (PD).
The transformation from a disease affecting six people in London to one affecting six million (and now nearly 12 million people) cannot be explained by genetics alone. Human genes don’t change significantly over 200 years. Nor can increased longevity fully account for the rise, as PD is growing faster than can be explained by aging and much faster than other age-related brain diseases like Alzheimer’s and stroke.
PD is not a natural consequence of aging, Dr. Dorsey said. A mouse in a laboratory will never spontaneously develop PD as it ages, nor will it develop Alzheimer’s. The only way that a mouse develops PD is if researchers manipulate its genes or expose it to toxic chemicals. PD is an unnatural consequence of aging.
In “The Parkinson’s Plan,” Dr. Dorsey and co-author Dr. Okun argue that the principal causes driving this transformation are environmental chemicals. These include pesticides (in food, water, and air), degreasing and dry cleaning chemicals like TCE (in water and air, particularly in areas like Silicon Valley), and outdoor air pollution. Exposure can occur through ingestion, inhalation, or direct contact with the skin.
The Genetics Question
Only about 13% of Americans with PD carry any known genetic cause or risk factor for the disease. Put another way, 87% of Americans with PD don’t carry any genetic cause or genetic risk factor. The principal causes of the disease do not lie within our DNA but outside of us in our environment.
Dr. Caroline Tanner (currently at the University of California San Francisco and LA VA) published a twin study in JAMA in 1999 about genetic contributions to the disease. Twin studies work on the principle that if something is very genetic, identical twins would be much more likely to share the disease than fraternal twins. She found no difference. Identical twins and fraternal twins were both equally likely and equally unlikely to have PD, indicating the disease is predominantly not due to genetics, though there was a small signal suggesting identical twins under age 50 were slightly more likely to share the disease.
The Rostock study in Europe examined about 10,000 individuals with PD across Europe, North and South America, and the Middle East. It found that 14% of people with PD carried a genetic cause or genetic risk factor, very similar to the 13% figure for the United States. Among people diagnosed under 50, 20% carried a genetic cause or risk factor. For those under 30, 30% carried a genetic cause or risk factor.
Said another way, if someone has an age of onset under 30, 70% of people with PD have no known genetic cause or genetic risk factor for the disease.
Young Onset Parkinson’s
The rise in young onset PD is particularly telling. If it’s rising and it’s young, it can’t be explained by aging. It’s difficult to explain by genes. Dr. Dorsey believes environmental exposures are the cause.
The book profiles Dr. Jana Reed, who attended one of the local talks, and Dr. Sara Whittingham. Both graduated from the Air Force Academy where they ran track. Both became physicians, served their country in Afghanistan, and became mothers. Both were diagnosed with PD within one month of each other in their 40s.
Diseases Have Causes
Dr. Dorsey emphasized a fundamental principle of Western medicine: diseases have causes. “Diseases come and go,” he said. “Diseases are not permanent features of human society.” Early humans died from different diseases than modern humans. People no longer die of typhus, yellow fever, polio, or smallpox. Dr. Dorsey pointed to other diseases that have been eliminated or dramatically reduced: cancer of the scrotum among chimney sweeps, once common, is now in textbooks but not affecting humans.
Once we identify the causes of diseases, we can create a world where those diseases become increasingly rare.
Trichloroethylene (TCE): The Key Chemical

About eight years ago, Dr. Dorsey was introduced to trichloroethylene by Dr. Tanner (from UCSF and the SF VA). TCE has been used to degrease metal and dry clean clothes for a century. It was widely used in Silicon Valley to clean silicon wafers.
The chemical’s structure consists of six atoms: two carbon atoms, one hydrogen atom, and three chlorine atoms (hence the name “trichloroethylene”). It has a cousin called perchloroethylene (or PCE, also called tetrachloroethylene), which has the same structure but with a fourth chlorine atom instead of the hydrogen.
In 1970, an estimated 10 million Americans, including many in Silicon Valley, worked with this chemical. It was used to clean carpets, clean guns, in typewriter correction fluid, and to decaffeinate coffee. The most recent data showed about 250 million pounds still being produced annually. In 1970, 500 million pounds (about 2 pounds per American) were used.
People can be exposed to TCE through work or through environmental contamination. The chemical contaminates up to 30% of groundwater in the United States.
Superfund Sites and Silicon Valley
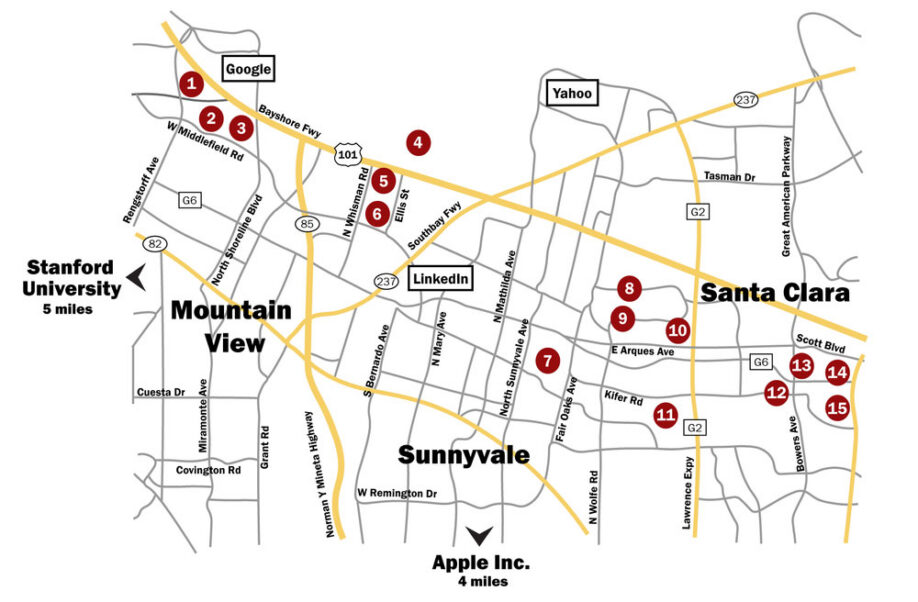
Superfund sites are the most toxic sites in the country, designated by the federal government for cleanup. Love Canal was the first Superfund site. Silicon Valley has 15 of the approximately 1,500 Superfund sites in the United States. Eleven are located on a seven-mile stretch of Highway 101.
Dr. Dorsey mentioned Jane Horton, who lives in Mountain View, California, next door to one of these Superfund sites. TCE, known to cause cancer and associated with a 500% increased risk of PD, was present in the indoor air of her home. The chemical can evaporate from soil and groundwater, similar to how radon evaporates from soil and enters homes to cause lung cancer. TCE can evaporate from groundwater or soil, enter homes, and cause both cancer and likely PD.
After having her home tested and finding TCE present, Horton had a remediation system installed that sucks air from underneath her foundation and vents it above her roof. Horton, who attended one of the local events, says, “I have the cleanest indoor air in all of Mountain View, California.”
People living near these contaminated sites often have no idea the chemical could be in their indoor air. They could have been breathing it in for years without knowing.
How TCE Enters the Environment
The chemical enters the environment through several pathways:
- Leaking from underground storage tanks and drums
- Leaking sewer lines or disposal lines
- Inappropriate disposal (often simply poured onto the ground)
- Disposal from automobile mechanic shops
- Disposal from dry cleaning sites
- Disposal from jet engine maintenance sites
A high school in Oakland, California had TCE in their indoor air.
Current Status of TCE Use
The EPA banned TCE use in 2024. However, in 2025 that ban was frozen. The ban calls for a phase-out over the next 10 years, so TCE is still being used in the United States.
California is the only state in the U.S. that has banned the use of perchloroethylene (the cousin chemical with four chlorine atoms) for dry cleaning. Dry cleaners in California are not allowed to use it, but it continues to be used elsewhere.
TCE should be out of household products now, but people with old products in garages might still find it in gun cleaners, carpet cleaners, and photography chemicals. Some people worked with it as teenagers in photography clubs, spending years in darkrooms with the chemical.
The Evidence Linking TCE to Parkinson’s
Dr. Tanner (at UCSF) and her colleague Sam Goldman, MD, looked at twins from World War II, examining hobby and occupational exposure. People who either worked or engaged in hobbies with TCE had a 500% increased risk of PD compared to their twins who did not have such exposure.
At Marine Corps Base Camp Lejeune, where TCE contaminated the drinking water from 1953 to 1987, Dr. Tanner and Dr. Goldman found that Marines who served there had a 70% increased risk of developing PD compared to Marines who served at a different camp in southern California. In the latter years, the Marines knew there was a cancer-causing chemical in the drinking water exposing the best and brightest Americans and didn’t do anything about it.
Marine officers needed dry-cleaned uniforms, and the dry cleaner near the base inappropriately disposed of the chemical, contaminating the groundwater. The base was like a college campus, exposing not only Marines but also their families, children, and all civilians who worked there. An estimated one million people were exposed. Former basketball player Brian Grant, who played for the Portland Trail Blazers, was a three-year-old boy when his father was a Marine stationed at Camp Lejeune. He was drinking the contaminated water and 33 years later developed Parkinson’s disease. In laboratory studies, TCE reproduces the features of PD both when examining animal brains and when observing disease symptoms. Both laboratory and epidemiological studies link the chemical to PD.
Dry Cleaners and Parkinson’s Risk
A study conducted in Denmark asked which occupations had the highest risk of PD: attorneys, accountants, retail clerks, manufacturers, or dry cleaners? The occupation with the highest risk was female dry cleaning workers, with a 1,500% (15-fold) increased risk. The study was small, with only three individuals affected when zero to two were expected.
For comparison, smoking’s link to lung cancer is a 30-fold risk; TCE’s link to PD is a 15-fold risk.
Paraquat: Another Dangerous Chemical
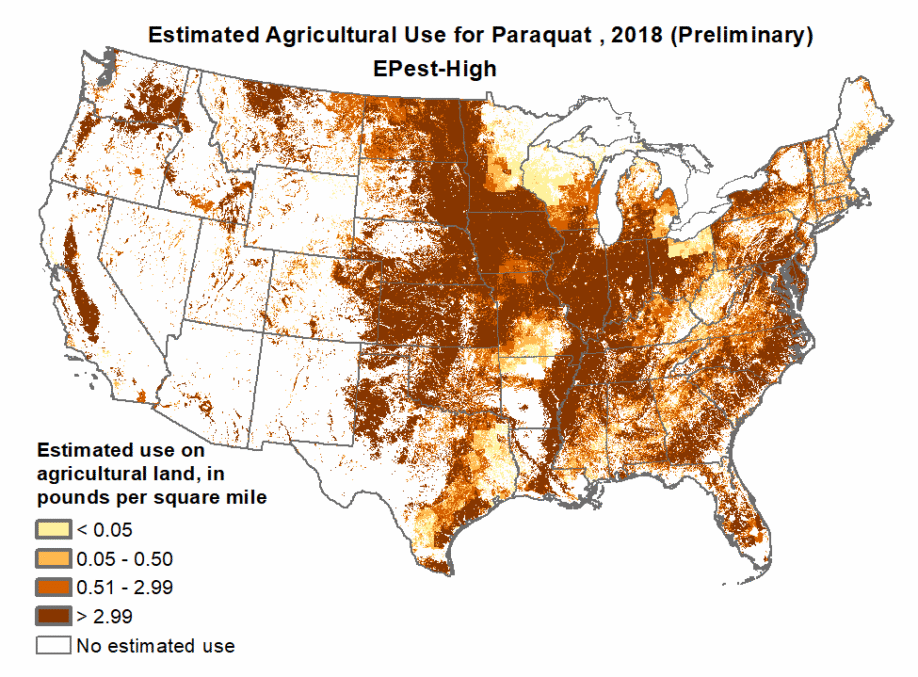
Dr. Dorsey discussed paraquat, a weed killer banned in 50 countries including the UK and China (where it’s manufactured), yet it remains one of the most widely used herbicides in the United States.
A UCLA study of Central Valley (California) residents found that people exposed to paraquat had a 250% increased risk of developing PD. Paraquat is named for its chemical structure, which looks similar to a chemical used to induce PD in laboratory animals. It damages the same part of the brain affected in PD (the substantia nigra) and kills the same dopamine-producing nerve cells that die in PD.
Paraquat is so toxic that a small sip of the concentrated version (about a tablespoon) is often fatal. It’s dyed blue to distinguish it from beverages and has an added chemical to induce vomiting if ingested. Workers are required to wear full-body protection when handling it, yet it’s sprayed widely across U.S. farmland.
Air Pollution’s Impact
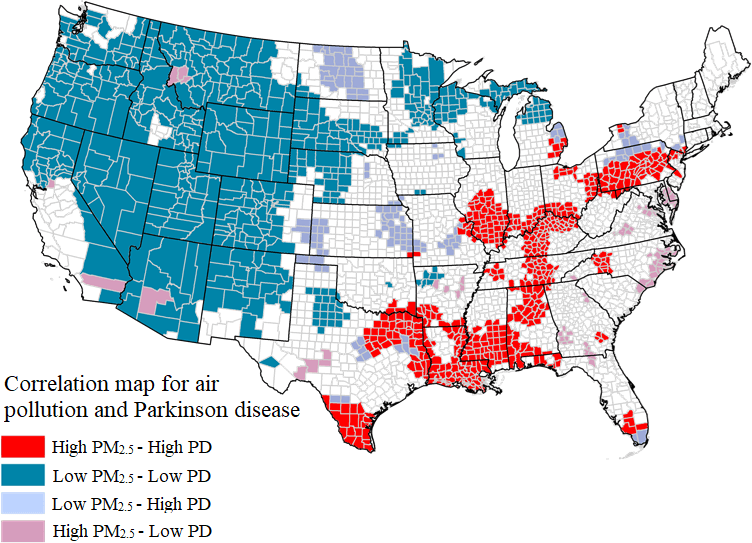
Air pollution costs humans on average three years of life. According to the Global Burden of Disease study, air pollution is more disabling than high blood pressure.
Small pieces of dirt and soot in air pollution (technically referred to as PM2.5, meaning particulate matter sized 2.5 micrometers or less) are so tiny they can penetrate the olfactory nerve (responsible for smell) in the upper nasal passages. They act like a Trojan horse, bringing toxic metals including lead, iron, and platinum into the brain. People with PD and Alzheimer’s can have high levels of iron in their brain; the exact reason remains unclear. Dr. Dorsey expressed concern that air pollution plays a role.
To avoid dementia and Alzheimer’s, minimizing exposure to air pollution is critical. It’s never too late. The Nurses’ Health Study followed nurses who were on average 74 years old with normal cognition at baseline. Those living in parts of the country with poor air quality had greater cognitive decline over the next eight years compared to those living in areas with clean air.
Two Pathways: How Parkinson’s Begins and Spreads
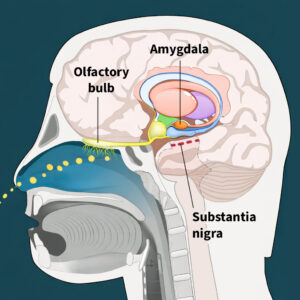
When an audience member asked about protein misfolding and whether PD damage spreads from cell to cell, Dr. Dorsey explained how environmental chemicals contribute to the disease process. All these chemicals (paraquat, pesticides, TCE, air pollution) damage the mitochondria, the energy-producing parts of cells. The brain is only 2% of body weight but consumes 20% of the body’s energy. The dopamine-producing nerve cells lost in PD have enormous energy demands because they’re surprisingly large (four meters in length if stretched out, twice Dr. Dorsey’s height), have a million connections, and aren’t insulated. The chemicals damage mitochondria and contribute to the misfolding of a protein called alpha-synuclein.
In 2003, German pathologist Heiko Braak challenged the assumption that PD is primarily a brain disease. Looking under the microscope, he found the disease begins in nerve cells near the nose (responsible for smell) and in nerve cells that go to the gut via the vagus nerve. He theorized that PD might begin in the gut and spread like dominoes through the vagus nerve, potentially causing early constipation, then affecting parts of the brain responsible for sleep (causing sleep disturbances), and eventually reaching the part responsible for tremor and slowness of movement.
In 2019, Dr. Per Borghammer in Denmark built on Braak’s work and proposed two distinct forms of PD: a gut or body-first form and a nose or brain-first form. The body-first form begins in the gut, where the misfolded protein spreads from nerve cell to nerve cell, producing more symptoms as it spreads up toward the brain. A nose or brain-first form begins in the smell center (loss of smell is often an early symptom), makes one stop in the amygdala (potentially causing depression and anxiety), before reaching the substantia nigra (causing tremor and slowness of movement).
Dr. Dorsey proposed to Dr. Borghammer that ingested chemicals might cause the gut-first form while inhaled chemicals cause the nose-first form. Though initially skeptical, Dr. Borghammer agreed the hypothesis made sense, and they co-authored an article on the connection.
Examples: Marines drinking contaminated water at Camp Lejeune or people drinking pesticide-contaminated well water might develop gut-first PD, while people breathing TCE in their home might develop nose-first PD.
Dr. Borghammer believes most PD (about two-thirds) begins in the nose as a brain-first disease. About two-thirds of dementia with Lewy bodies (which presents with parkinsonian features, dementia, and hallucinations) begins in the gut..
Evidence that misfolded protein spreads from nerve cell to nerve cell comes from stem cell therapy trials conducted about 20 years ago. Scientist Jeffrey Kordower examined brains of people who had received fetal stem cell transplants that developed into dopamine-producing nerve cells. Under the microscope, these healthy transplanted stem cells had the misfolded protein in them, suggesting the pathology had spread from sick nerve cells to healthy ones. Laboratory experiments have confirmed this protein can spread from nerve cell to nerve cell, a phenomenon also seen in Alzheimer’s, likely in ALS, and in disorders like mad cow disease.
Some of the 25 Steps to Prevent and Slow Parkinson’s
The book outlines 25 steps divided into five categories of five steps each. He discussed a few of them, summarizing the key points.
Avoid Chemicals

- Wash produce, even organic at least thirty seconds in water
- Avoid exposure dry cleaning chemicals, avoid living in proximity to dry cleaning facilities; find a “green” dry cleaning service
- Avoid paraquat and other harmful pesticides, buy organic when possible, especially berries, grapes, and leafy greens
- Avoid TCE and related degreasing agents, dispose of old products containing TCE safely
- Filter your water – Especially important for well water users; consider reverse osmosis systems
- Improve indoor and outdoor air quality. Use air purifiers; monitor air quality
- If you live near a golf course or spend a lot of time on the links, ask course management: what pesticides they use, to avoid using 2,4-D or chlorpyrifos, to spray less frequently in smaller amounts, and to provide advance notice to residents before spraying
Dr. Dorsey uses a small monitor to measure particulate matter in his indoor air, comparing it to having a thermostat for temperature. Air quality is likely more important for health than temperature. He bought an air purifier after moving to New York City.
Wildfire smoke is a significant concern. Given what’s been learned about wildfire exposure, air purifiers should be at the top of the list for California residents.
Eat Healthfully
The recommendations follow a Mediterranean diet:
- Eat more plants
- Consume good fats (Mediterranean diet)
- Reduce caloric intake when possible
Exercise Regularly

This is perhaps the most important intervention for people with PD. Dr. Dorsey stated that if he had PD, he would exercise two hours daily.
Exercise may help protect nerve cells from toxic chemical effects. There are several theories about exercise’s benefits:
- It may increase brain-derived neurotrophic factor (BDNF), which supports nerve cell health
- It may help clear toxic proteins
- It improves cardiovascular health, which affects brain health
For people experiencing fatigue after exercise, Dr. Dorsey suggested:
- Taking levodopa about 30 minutes before exercise to help with movement
- Taking naps (30-60 minutes, ideally not much longer) as “the best treatment for fatigue”
- Using caffeine for daytime sleepiness, though it’s less effective for fatigue itself
Sleep Well
Quality sleep is essential for brain health and may help clear toxic proteins from the brain.
Reduce Stress
Chronic stress affects overall health and may influence disease progression.
Additional Specific Recommendations
Coffee and Caffeine
Caffeinated coffee appears protective. Caffeine may protect nerve cells from toxic chemical effects. The benefit appears to come from the caffeine itself, not the coffee, so other caffeinated beverages like tea are likely beneficial as well. This is one of the few recommendations that Dr. Dorsey personally doesn’t follow.
Alcohol
While alcohol clearly harms brain health broadly, there’s no evidence it directly causes PD. However, Dr. Dorsey would probably recommend minimizing alcohol exposure as a potential “26th step” because it’s not good for brain health in general and is likely especially problematic for people who already have a neurological disorder.
Water Testing and Treatment
For municipal water users: While the Safe Drinking Water Act (1973) requires regular testing and monitoring, municipalities don’t test for many chemicals, and standards become stricter over time. Dr. Dorsey recommends staying ahead of the curve by using water filters even with municipal water. He uses a water filter in New York City and did so in Rochester.
For well water users: Private wells are not regulated by the Safe Drinking Water Act. They’re infrequently tested, usually only when buying or selling a home, and typically tested only for bacteria, not pesticides or TCE/perchloroethylene.
Recommendations for well water:
- Test for pesticides if in an agricultural area
- Test for TCE if in an industrial area
- Use water filters regardless (100% recommendation)
- Consider reverse osmosis systems for under-sink installation
- Companies like Simple Labs offer testing (Dr. Dorsey has no financial ties to any testing companies)
Home Chemical Testing

People should check old containers of chemicals in garages for TCE. It was used in gun cleaners, carpet cleaners, and products for cleaning engines. When engines were sprayed and grease melted away, that was TCE.
Air Quality Monitoring
Dr. Dorsey recommends monitoring indoor air quality just as people monitor temperature with thermostats. He purchased a monitor to measure particulate matter when he moved to New York City, even though the air quality was fine, and then got an air purifier. For California residents, given wildfire concerns, an air purifier should be a top priority.
PD Avengers and Research
Dr. Dorsey mentioned PD Avengers (pdavengers.com), a global grassroots organization founded and run by people with the disease. People can sign up to participate in future research studies measuring these chemicals in people’s bodies and environments. The goal is to take action to reduce chemical exposure in bodies and environments to help create a world without these terrible diseases.
The new Atria Center for Brain and Environment in New York City focuses on identifying root causes of brain diseases from autism to Alzheimer’s so they can be prevented.
Taking Action
Dorsey emphasized that changing the course of disease requires people making their voices heard. “You don’t need to go back too far in history,” he said. In the 1980s, activists in San Francisco changed the course of HIV. Forty-five years ago, Candace Lightner changed the course of drunk driving in California after her 13-year-old daughter was struck and killed by a drunk driver. Lightner petitioned Governor Jerry Brown every day for a year, leading California to make drunk driving illegal, raise the drinking age to 21, and drop the blood alcohol limit to 0.08.
In 1998, Roina Su dropped off her kindergartner Nicholas at Sherman Oaks Elementary School in Los Angeles. As he turned to kiss his mother goodbye, he encountered a cloud of weed killer sprayed by a man in a hazmat suit. Nicholas said it tasted terrible and began to wheeze. When he asked if this would happen again, his mom said no. Two years later, spurred by her activism, the California legislature passed the Healthy Schools Act, requiring K-12 schools and childcare centers to minimize chemical use, ban high-risk pesticides on schools and surrounding parks, and notify parents annually if pesticides are used.
“So when people like you say no to paraquat, no to toxic pesticides like 2,4-D and chlorpyrifos on our golf courses, no to pesticides on sports fields,” Dr. Dorsey said, “we create a world where these diseases start to disappear. Just like we don’t have typhus, we don’t have yellow fever, we don’t have smallpox, we don’t have cancer in the scrotum. The list of diseases that are in the textbooks but not affecting humans is long. We can add Parkinson’s disease to that list.”
Dr. Dorsey’s passion on this topic is deeply personal. “I get pissed off when I see you guys with Parkinson’s because I think you’ve all been robbed,” he said. “I see people robbed of their independence. I’ve seen people robbed of their incomes. I’ve seen people robbed of their profession. I’ve seen people robbed of being a mom … I’ve seen people robbed of their future retirement plans. I’ve seen families torn apart. I’ve seen all of it.”
The evidence from epidemiological studies, laboratory research, and real-world cases demonstrates clear links between environmental chemicals and PD. While some call for more evidence, Dr. Dorsey believes “we’re just asleep” to what we already know.
The goal is not just to treat PD but to prevent it by eliminating exposure to the chemicals causing it. This requires both individual action – filtering water, buying organic, using air purifiers – and collective action – banning harmful chemicals, cleaning up contaminated sites, advocating for policy changes.
(End of the notes from Dr. Dorsey’s two talks)
Links to help follow some of Dr. Dorsey’s recommendations:
- Search for Superfund Sites Where You Live (EPA)
- Silicon Valley Superfund sites (Ending Parkinson’s)
- 7 Tips for Cleaning Fruits, Vegetables (FDA)
- Region 9 (Pacific Southwest) (EPA)
Research papers mentioned by Dr. Dorsey:
- Parkinson Disease in Twins: An Etiologic Study Caroline M. Tanner, Ruth Ottman, Samuel M. Goldman, et al. JAMA, 1999
- The Body, the Brain, the Environment, and Parkinson’s Disease E. Ray Dorsey, Briana R. De Miranda, Jacob Horsager, Per Borghammer Journal of Parkinson’s Disease, 2024
- Neuropathological Evidence of Graft Survival and Striatal Reinnervation after the Transplantation of Fetal Mesencephalic Tissue in a Patient with Parkinson’s Disease Jeffrey H. Kordower, Thomas B. Freeman, Barry J. Snow, et al. New England Journal of Medicine, 1995
- Risk of Parkinson Disease Among Service Members at Marine Corps Base Camp Lejeune Samuel M. Goldman, Frances M. Weaver, Kevin T. Stroupe, et al. JAMA Neurology, 2023