
In March 2026, the American Parkinson Disease Association (APDA) hosted a webinar titled “Staying Connected: Overcoming Communication Barriers.” Corinne Casey, SLP, and Anna Reeve, SLP, both speech-language pathologists from Lingraphica, said that communication changes are very common with PD and also very manageable with daily use and practice of communication strategies. When communication becomes more difficult, it can affect independence and daily functioning. The webinar is part of the APDA’s “Thriving Through Speech Therapy” series.
Key Takeaways
Communication is broader than speech. It includes tone of voice, facial expressions, gestures, memories, context, and connection. Parkinson’s affects expression (softer voice, slurred words, reduced facial expression), cognition (attention, memory, problem-solving), and reception (understanding others, monitoring your own speech). Communication breakdowns can result from changes in any one of these areas—or a combination of them.
A communication ramp is anything that makes it easier for someone with communication difficulties to understand others and express their thoughts. Similar to how wheelchair or accessibility ramps provide access to spaces, communication ramps provide support for successful communication. One person’s ramp might include short sentences, simple drawings, picture choices, or simply time to rest; ramps will look different depending on the individual and change over time.
Use the right tools for different moments. When speech is clearer, use intentional strategies (speak louder on purpose, pause between thoughts, exaggerate articulation). During downtimes (between medications, busy days, fatigue), use writing, gestures, pictures, voice amplifiers, speech-to-text apps, or dedicated communication devices. All forms of communication are valid.
Daily practice matters. A few minutes a day can make a big difference. Practice during real moments—chatting over coffee, making phone calls, talking with family. Pair practice with daily habits (commercial breaks, morning coffee, answering the phone). Aim for progress, not perfection. Be sure to celebrate wins, track your efforts, and get feedback from communication partners.
Stay connected to combat isolation. Connection boosts mood, supports brain health, provides natural practice, and reduces stress. Join support groups where people understand what you’re going through. Staying socially active is one of the most powerful things you can do.
Communication is a team sport. Make small shifts together—such as turn down background noise, sit face to face, offer yes/no choices when someone is stuck. Slow down, create space, give each other extra time. Acknowledge effort and progress. Plan important conversations during stronger times of day. Use hand signals for reminders. Ask “Do you want me to help?” and “Was that helpful or too much?”
Resources
Webinar Recording:
Watch on APDA YouTube Channel
Stanford Parkinson’s Community Outreach Resources:
Additional Resources Mentioned:
- APDA Printable Medical Cards
- Free Resources from Lingraphica (Their Parkinson’s Communication Toolkit including eBook “Navigating Communication Challenges in Parkinson’s”, Communication ID Card, Low-Tech Communication Boards)
Note: While the speakers are both paid employees of Lingraphica, a company that provides speech-generating devices and apps for people who have trouble speaking or communicating, the webinar was not an advertisement for their products.
Continue reading for a detailed summary of the webinar.
-Elizabeth
“Staying Connected: Overcoming Communication Barriers”
Speakers:
- Corinne Casey, MA, CCC-SLP, Clinical Consultant, Lingraphica (Cleveland, OH)
- Anna Reeve, MS, CCC-SLP, Manager of Clinical Relationships, Lingraphica
Webinar Host: American Parkinson Disease Association
Webinar Date: March 4, 2026
Summary by: Elizabeth Wong, Stanford Parkinson’s Community Outreach
Communication is More Than Just Speech
At its simplest, communication is an exchange of information. Most commonly, we think of communication as verbal speech—transfer of words to convey information. But communication is much broader and encompasses many factors: setting, tone of voice, context, facial expressions, memories, gestures, and much more.
When we think about this broader definition—exchanging information through tone, facial expressions, memories, gestures—the understanding of why Parkinson’s so significantly impacts communication becomes more clear.
Communication changes are very common with Parkinson’s and also very manageable with daily use and practice of communication strategies.
Three Parts of Communication Affected by Parkinson’s
Parkinson’s can affect multiple parts of the system at the same time:
1. Expression – Many people first notice changes here:
- Speech may become softer, hoarse, or breathy
- Words might come out in short bursts, sound slurred, or be harder to find
- Facial expression and body language may decrease
- Even nonverbal communication can change
2. Cognition – Communication is influenced by how we think and process information:
- Parkinson’s can affect attention, memory, and problem-solving
- Changes in mood, energy, or fatigue can make it harder to participate in conversation
3. Reception – How communication is perceived and understood:
- Some individuals have more difficulty understanding others, especially in complex or noisy environments
- Changes in sensory feedback—how we monitor the speech we produce ourselves
- Example: Someone may feel like they’re speaking really loudly (even yelling) when their voice is actually quite soft
When communication breakdowns occur with Parkinson’s, it’s rarely just one factor. It’s usually an interaction between expression, cognition, and reception. When we understand which parts are being affected, we can put the right strategies in place to support clearer and confident communication.
Why Communication Matters
When communication becomes more difficult, it can affect independence and daily functioning—from managing appointments to participating in conversations at home or in the community.
Over time, changes can impact a person’s sense of self and identity. Communication is how we share our personality, opinions, humor, and values. When expressing those things becomes harder, it can feel like losing a part of yourself.
Perhaps most significantly, communication breakdowns can lead to feelings of isolation. When conversations take more effort, some people begin to withdraw. Others may unintentionally start to speak for them. Connection becomes strained even when the desire to connect is still very strong.
This is why addressing communication in Parkinson’s is so important. It’s not just about volume or clarity. It’s about preserving independence, identity, and meaningful relationships.
What is a Communication Breakdown?
A communication breakdown occurs when there’s a disruption in the exchange of information—when a message expressed is not understood by the other person in the conversation.
When communication breakdowns occur repeatedly, they affect more than just the conversation itself. They impact emotional well-being, interfere with daily activities, and place strain on relationships.
Signs of Communication Breakdowns
Person with Parkinson’s may experience:
- Frustration
- Difficulty following conversation
- Not being understood
- People asking them to repeat themselves a lot
Family and friends may notice:
- More filler words
- Looking confused at times
- Repeating words a lot
Recognizing these early signs helps you adapt communication strategies quickly to avoid further frustration. By identifying when breakdowns are happening, you can intervene early.
Communication Ramps: The Right Level of Support
We’ve all seen accessibility ramps for people with physical disabilities—they allow access to public spaces and homes. There are communication ramps too. Communication ramps provide the support that leads to success for communication challenges. There’s so much we can do to make communication easier, and this is a group effort—not just something the person with Parkinson’s deals with alone.
What Communication Ramps Look Like
Your communication ramp isn’t just one thing—you’ll use several things that allow you to communicate with more ease. It’s about finding the right amount of support, not too much or too little.
Some individuals might have just a few things at first. Others might need many supports. Your ramp will look different from others.
Examples of communication ramps:
- Entering conversation with positive frame of mind
- Using short or simple sentences (either from communication partner for someone who has difficulty understanding, or from person with Parkinson’s to communicate more clearly)
- Simple drawings
- Providing picture choices or word choices
- Time in between to rest
Your communication ramp will change over time. It’s ultimately up to us to ask the individual: What helps you? What support do you need? What does your ramp look like?
Tips for Managing Communication Breakdowns
1. Be Prepared and Share Your Strategies
Sometimes it’s helpful to have a written copy of your strategies or communication ramps to share with others. If you have difficulty communicating, it makes sense not to have to explain to every single person what they can do to help. Sharing that information to friends and family so they can prepare on how to support you can be really helpful.
2. Advocate for the Right Level of Support
We’ve all interacted with somebody who wants to help a ton—maybe they’re interrupting, maybe they’re giving too much help. That can be frustrating in itself. None of us communicate our best when experiencing frustration.
Advocate for what you can do. This is about getting the right level of support and making sure you can be as independent as possible.
Mistakes are going to happen. Communication breakdowns are expected when you have a communication challenge. Every mistake is an opportunity to learn what works for you for the future.
3. Prepare and Plan Ahead
Work with your speech therapist to determine your specific strategies, how to communicate those strategies out to people, and if strategies aren’t working the way they used to, revise that plan.
Practice or role play your strategies outside of communication pressure. Not in the exact environment where you’ll use them, but in low-pressure situations.
Communication breakdowns can be more frequent when you’re tired, fatigued, or having a rough day. Take breaks and rest when possible—that will help you address breakdowns in a better way.
Resources and Tools
Voice Amplifiers: A personal voice amplifier can really benefit someone with Parkinson’s. A lot of people are just not loud enough, and this might fluctuate at different times of day. A voice amplifier is a nice way to boost your voice and reduce breakdowns if you can’t be successful with just increased effort or strategies.
APDA Printable Medical Cards: You can download these cards that explain why you’re having difficulty communicating. Not everyone knows what Parkinson’s is or would expect communication problems. Sharing something written can be helpful in educating your community and having them understand you might need a little more time. (Download here)
AAC (Augmentative and Alternative Communication): AAC can be really helpful for people who have a gap between what they want to say and what they’re able to say.
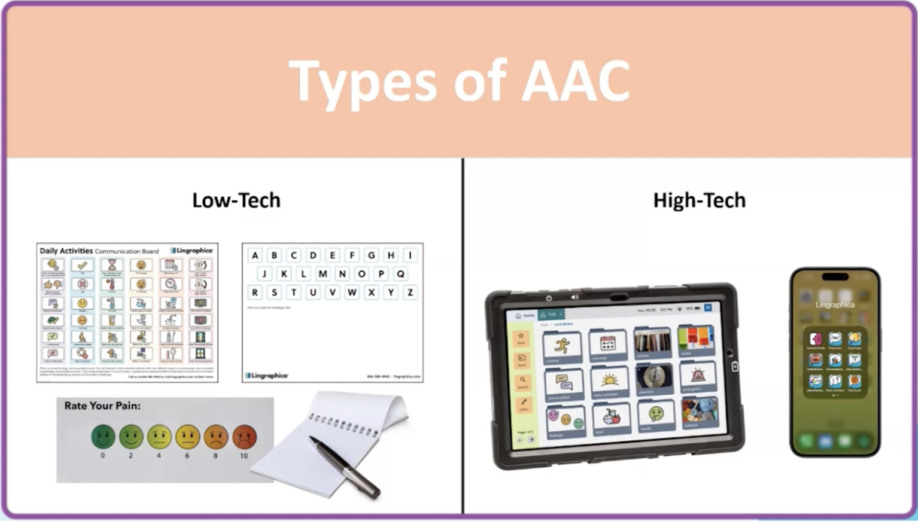
Low-tech options:
- Handwriting
- Pointing to pictures
- Communication boards
High-tech options:
- Dedicated AAC devices with voice output
- Apps on tablets/phones
- Voice output makes it easier to answer phone calls, get someone’s attention, talk from across the room
You might use different tools for different scenarios. It’s not one or the other—you might have a combination of these things to help throughout your day.
Free Resources from Lingraphica (Visit here)
- Ebook: “Navigating Communication Challenges in Parkinson’s” (free download)
- Join in Parkinson’s groups: Free social meetup groups that meet online over Zoom
- Communication ID card (free)
- Downloadable low-tech communication boards (free)
Overcoming Common Barriers
Barrier #1: Speech Clarity
The system your brain uses for intentional movement (when you think to do specific movements) doesn’t rely on dopamine the same way as when you have automatic movements. That means you can bring more purpose and attention to how you speak—you can often make your voice clearer and easier to understand.
Simple intentional strategies:
- Slow down a little bit
- Take a fuller breath before you start talking
- Be more deliberate with how you move your mouth or how loud you are
- Speak a little louder on purpose
- Pause between thoughts
- Exaggerate articulation
Yes, this means thinking about the process more. But these small shifts can make a real difference in whether you’re understood.
Important: It’s very common to need more reminders and different strategies over time. Regularly check in on what strategies you use and their effectiveness in day-to-day life.
Barrier #2: Downtimes
Between medication times, busy days, fatigue, illness, or progression of symptoms, you might notice moments where talking is more difficult. This is typical—expect it.
When you’re prepared, you learn that certain times of day you can speak clearly and use the strategies. Other times you may need other tools.
Other tools to use:
- Writing
- Gestures
- Pictures or drawings
- Voice amplifiers
- Speech-to-text apps
- Dedicated communication device
The more tools in your toolbox, the better. All communication forms are valid. Use what works right now. Be comfortable pulling different tools out when you need them. You’ll use different tools for different moments.
Barrier #3: Building New Habits
Learning new strategies and building new habits—especially with something we do every single day like talking—can be really hard. That’s true for all of us. A small, consistent plan, even just a few minutes a day, can make a big difference. Focus on progress, not perfection. Celebrate moments that work versus where you struggle.
Daily Practice Suggestions:
- Carve out routine practice at same time each day:
- Read aloud using your strategies
- Sing if you enjoy that
- Do exercises assigned from speech therapist
- Pair speech practice with daily habits:
- Morning coffee
- Commercial breaks during favorite shows
- Answering the phone
- Specific times of day where you focus on new strategies, then slowly incorporate into every communication
- Get feedback from communication partners: Family and friends communicate with you most. Have check-ins: “Are you hearing me okay? Do you hear me using these strategies?” Get feedback on when you’re doing great and when you need more reminders.
- Accountability buddy: Track which days you’re practicing (maybe in journal). Notice small changes. Maybe you forgot some days, but last week you did it 3 days in a row, next week you did 5. Celebrate those wins—that’s motivating.
Barrier #4: Isolation
People with Parkinson’s can feel really isolated. Reduced dopamine also has impacts beyond movement. Staying connected can take effort, but it’s one of the most positive and powerful things you can do for your own well-being.
Why connection matters:
- Boosts mood
- Supports brain health
- Gives real motivation to keep practicing communication strategies
- When around other people, you’re forced to practice (natural practice vs. practicing alone)
- Boosts cognitive function through social interaction
- Reduces stress and anxiety, especially with people who understand what you’re going through
- New conversations are cognitively stimulating
This isn’t just for people with Parkinson’s, but also for caregivers. They need time to talk with others, share experiences, and feel supported.
Options to stay connected:
- Speak Out! home practice sessions (Parkinson Voice Project)
- Join In Parkinson’s virtual community (Lingraphica, free, register in advance)
- Michael J. Fox Foundation Parkinson’s Buddy Network
- Local community support groups or senior activities
- Maintain social activities you’re used to doing
- Engage in small talk wherever you go (communication practice)
- Become a Parkinson’s ambassador: speak at local support groups, volunteer for peer support, educate communities about Parkinson’s
It’s okay if one option isn’t a good fit—try starting with one. There are lots of resources and organizations offering different options.
Managing Cognitive Changes
If you’re noticing cognitive changes—difficulties with thinking, memory, or attention—talk to your doctor. This can happen at different times in the disease process. They can diagnose and make referrals as appropriate (which might be to see a speech therapist). They can also provide medications that might reduce symptoms or maintain what you have currently.
If noticing safety considerations, memory issues, or judgment problems, those conversations are also really important to have with your doctor.
A speech therapist can:
- Identify strengths and weaknesses (through evaluation or asking questions about how things are going at home, chatting with caregivers)
- Teach cognitive strategies and support ways to mitigate changes and reduce their impact on day-to-day life
- Provide suggestions for stimulation and structure to routines so you can be more successful
- Goal is always to improve independence and maintain whatever you can do
Things You Can Do
- Reduce stress and cognitive load: Stress impacts memory and attention. If you have a lot on your mind or are dealing with stress, it’s harder.
- Focus on activities you value: Have conversations with family about what you feel strongly about continuing versus what others could do. This can reduce stress and errors.
- Have open conversations with your team: Build insight and awareness as to what others are seeing, what’s possible, what your options are. Don’t shy away from this—many people struggle with it.
Cognitive Support Tools (Communication Ramps for Cognition)
These are meant to support you so you can continue to do what you’re able to do with success.
Options:
- Verbal or visual reminders
- Increased care and support
- Tracking changes and discuss with doctor or therapist
- Counseling can help individuals understanding what is happening to their body and coping strategies can help
External Aids
- Smart devices – Reminders (people use these in general, not just people with cognitive challenges)
- Written and visual aids
- Talking medication boxes – Remind you when to take medications
- Hearing aids – Super important if you wear them, wear them consistently
Research shows: People with hearing loss are at increased risk for cognitive changes as they age. That ambient noise and stimulation we’re constantly getting—people with hearing loss aren’t getting that if not wearing hearing aids. Wearing them can improve cognitive function and certainly improve communication.
Medical and Lifestyle Factors
Talk with your doctor about:
- Medication adjustments
- Exercise
- Diet
- Addressing sleep issues
- Addressing depression
Sometimes depression can appear like a cognitive challenge. When medical doctors treat depression, sometimes memory and attention improves. Other things can mask and look like cognitive deficits that are truly other problems—they just have shared symptoms.
Self-Reported Scales
Physicians and therapists sometimes use “self reported scales”, also called “patient-reported outcome measures”. These are specific questions rating yourself on how you’re doing with specific areas.
Benefits:
- Can be self-rating or someone near you fills it out
- Tracks changes
- Sometimes we don’t think of every question we could be asking
- Reading through the scales could help one realize “I really do have hard time with organization”
- Calls out things and draws your attention to them
Establish Routines
Have routines and provide written aids that are out and visible showing what routines are—you’re not relying on memory to recall. Having that laid out step-by-step can help the day go smoother and reduce stress.
Using Family and Friends for Support
Communication changes affect family and friends deeply as well. This is an adjustment for everybody, and it’s okay to recognize that. It takes time, practice, and a lot of compassion on both sides. Even though communication may look different, connection is still very much possible. You, as family and friends, play a really powerful role in that.
Communication is a team sport. It is not solely the responsibility of the person with Parkinson’s to fix their speech. When both people make small shifts, conversation becomes less stressful and more successful. Reassuring your loved one that you’re there to help, not to rush them, can immediately reduce anxiety.
Ask:
- “Do you want me to help?”
- Afterwards: “Was that helpful or too much?”
This helps you find the right level of assistance. It also keeps dignity, respect, and independence in the communication exchange.
Sometimes having shared signals established ahead of time prevents frustration and keeps communication respectful.
- Hand gesture that means “I need a break”
- Hand gesture that means “Please repeat that”
Simple Changes That Help
- Turn down background noise
- Sit face to face
- Offer yes/no choices when someone is stuck
- If you don’t understand something, it’s okay to say so—say it gently though. Pretending to understand often leads to more isolation later. When both parties work together and make small adjustments, communication becomes easier.
Encouraging Communication Without Adding Pressure
When someone is working harder to get their message out, it’s natural to want to help—to jump in, to correct, to move conversation along. Most of the time this comes from a good place of love and care. But in practice, slowing down, creating space, and giving a little more time is often more helpful. This makes communication feel more manageable.
What helps:
- Extra time
- Patience with pauses
- Offering choices instead of open-ended questions
- Acknowledge the effort someone is putting in. Progress happens in small steps. Noticing changes can build confidence over time (for both people with Parkinson’s and family members).
Be specific with feedback:
- “I really liked the way you supported me there”
- “I heard you use those clear speech strategies—that really helped me understand you”
Gentle cues can help:
- “Hey, take a breath”
- “Can you try that again?”
- As long as they’re supportive and not rushed
What we’re aiming for is not perfect speech. It’s communication that feels successful enough that everybody involved wants to keep participating.
Early Recognition and Proactive Support
Communication changes happen gradually over time. Recognizing them early matters. Early support helps maintain communication skills, reduces frustration, and lowers risk of withdrawing from conversations or social activities.
Taking a proactive approach—responding to small communication changes early instead of waiting until they become a problem—leads to better outcomes in the long term.
Many times it’s the people around someone who notice first subtle changes:
- Slightly softer voice
- More difficulty finding words
- Conversation feeling more effortful
It’s really important to bring those observations to the attention of the person with Parkinson’s and their medical providers so strategies and support can be put in place right away.
Questions and Answers
Q: A person with Parkinson’s asked what to do when the care partner can’t wait for you to find the correct word or take time to take a deep breath? What advice do you have for how the person with Parkinson’s can approach that conversation with their care partner?
A: That’s very common. I usually acknowledge the care partner’s intent. I’ll say, “I know you’re trying to help them. Let’s give them a little bit more time” or “let’s have you count to 10 before you actually jump in and help.” I think it’s important for care partners to know the strategies that really help the person with Parkinson’s. It’s helpful to write down what your strategies are, what you do, and what kind of support you want from the other people. Therefore, your care partner doesn’t have to guess what to do at the moment. You can show them your strategies written down so they know what you want them to do to help.
Q: A person with Parkinson’s said I have difficulty comprehending what people say to me when they’re talking fast. Sometimes, when I’m reading something, it takes my mind a moment to catch up. Do you have any suggestions?
A: Be an advocate for yourself. If you have to ask that person five times to please slow down and give you more time, do it. Share what supports help you. Ask people to write down their messages. If you’re stronger with reading than listening, use speech-to-text software—most phones have it on the keyboard where you can click and record and it’ll transcribe what’s being said so you get that visual information too. I encourage people with auditory processing difficulties to focus on key words. There’s a lot of fluff in our language. If you focus on key words that are really sticking out, you can reduce the cognitive load of trying to process the entire message. You can also ask them to write down just the keywords so you can really soak in the message.
Q: We have had a couple of questions about the expiratory muscle strength trainer (EMST) and how that can help with speech and swallowing.
A: That’s a great resource that I use quite a bit in therapy. Talk to your doctor and speech therapist about it first—there are medical reasons why some people shouldn’t do this exercise because it involves holding your breath and doing effortful work. It’s a handheld device that your speech language pathologist can show you how to use. It’s proven to strengthen swallowing muscles and cough strength. Swallowing problems can be part of Parkinson’s disease, and when things go down the wrong pipe, you want a strong cough to expel it from your lungs. Speech therapists sing the praises of EMST because it can make huge changes in how people are able to cough, but make sure you clear it with your doctor and SLP first.
Q: A care partner asked for strategies that help keep the dignity of her person with Parkinson’s in mind. She says she doesn’t want to nag, but she wants him to be heard.
A: Check-ins are helpful. They may not want you to chime in when they’re talking with friends, but may welcome your reminders when they’re with family. You don’t have to correct it every single time you see it—just read the situation and check in with the person to make sure they’re open to your advice. Hand signals can come in handy because you’re not calling direct attention to it in a social situation. It’s a shared sign that only means something between you two. If he sees that visual gesture, he has the choice to acknowledge it or ignore it without disrupting the conversation.
Q: A person with Parkinson’s asked, what do you do when you are speaking and then you start stuttering? How can you regroup and continue?
A: That’s going to be very different depending on the individual. I’ve seen different strategies work for different folks, so I don’t want to give you a suggestion without knowing your specific situation. If this is increasing in frequency and you’ve seen a speech therapist, I’d encourage you to go back and reevaluate—see if the same strategies work or not. Medications and side effects from treatments like deep brain stimulation can cause this. Some people have persistent difficulties with stuttering and some don’t, so I’m cautious making suggestions without your particular situation.
Q: Can medication help or hinder stuttering, slurring words and voice issues?
A: It is very dependent on the medication and your medical situation. I recommend having a conversation with your medical provider or your pharmacist to get a better understanding of the side effects of your specific medication list.
Q: A care partner says their loved one has Parkinson’s with dementia, so they’re noticing speech issues caused from both the Parkinson’s and the dementia, and they’ve asked for any tips on how they can help facilitate communication with their loved one.
A: When somebody has a lot of cognitive challenges, we have to change our expectations. We want it to be enjoyable and play up on their strengths. We don’t want people frustrated. There’s not much purpose in correcting people or reminding them of something they’ve forgotten. Think about what you can do together that would be enjoyable and how you can figure out what they want.
Communication aids—either low-tech or high-tech—are often used with support. Sometimes people think “my loved one couldn’t use something like that,” but oftentimes it’s something you’re going to use together to figure out what they’re trying to say and what they want. Some people might need something written or with pictures because of an understanding problem or recall problem. If you provide choices, they can participate and you can go have a nice lunch together and enjoy yourselves. Look at what you can offer them that allows them to still make a choice and communicate something to you.
Sometimes with dementia, it can be really helpful to focus on things in the past—talking about reminiscence, playing familiar music, looking at old pictures. These things can open the door and make communication feel more achievable. It doesn’t need to be talking about what happened yesterday. Maybe look back at pictures from when the kids were younger or that one really awesome trip you took. Playing old music, especially from the teenage years, tends to bring more clarity. Play to those strengths and center the conversation around things that are still obtainable.