

In April 2026, Dr. Nate Komer, a doctor of physical therapy, presented a detailed look at gait and Parkinson’s disease (PD) for a Northwest Parkinson’s Foundation (NWPF) webinar. Gait changes are among the most common and consequential effects of PD, and understanding what causes them is important for addressing them. For people living with PD, walking and gait require attention and effort. For most of those without PD, walking is done without thinking.
The session covers the fact that dopamine loss causes gait changes in PD, how cognitive changes and anxiety impact walking, and the brain’s tendency to underestimate how much effort movement actually requires. Komer discusses three distinct gait patterns – bradykinetic gait, shuffling and festination of gait, and stiff-armed gait – explaining each case and what can be done about it.
Dr. Komer’s strategies range from simple home techniques –heel-strike cueing, counting steps, painters tape on the floor, breath control during freezing –to clinical approaches – forced-use treadmill training and visual cueing systems. He also discusses assisted devices, explaining why the right choice varies by person and why a walker is not always the safest option. The session closes with a look at emerging wearable technology, including smart shoes that use vibration to cue bigger steps, tracking socks, and robotic hip and leg devices.
Now, on to my detailed notes. – Kevin
Gait and Parkinson’s Disease
Speaker: Dr. Nate Komer, DPT, owner and founder, Parkinson’s Fitness Project, Seattle and Bellevue, WA
Webinar Host: Northwest Parkinson’s Foundation
Date: April 21, 2026
Summary by: Kevin Boyd, Stanford Parkinson’s Community Outreach
Why Gait Matters
Most people should take around 7,000 or more steps per day. People with Parkinson’s disease (PD), even those newly diagnosed, generally walk far less, around 5,000 steps a day or fewer. This decline in daily steps often goes unnoticed. A 2012 study tracked people with early PD through pedometers. Every few months study participants were assessed clinically. Even when doctors didn’t perceive physical changes and patients didn’t report them, step counts declined. There was a nearly 11% drop in steps per day year over year. Someone walking 5,000 steps at the start of the study was down to about 4,500 the following year. That kind of compounding decline has real consequences for overall health, strength, and independence. It may not be the disease alone driving physical deterioration, but the reduction in movement itself.
What Causes Gait Changes in PD
Dopamine loss is at the root of gait changes in PD. Dopamine is the neurotransmitter responsible for smooth, accurately sized movement. Without enough of it, movement becomes smaller, slower, and more rigid. Dopamine and acetylcholine normally balance each other in the brain. Dopamine drives smooth, fluid movement; acetylcholine, a neurotransmitter involved in muscle contraction and motor control, drives stability and rigidity. As dopamine production declines, the normal balance between the two neurotransmitters shifts. Acetylcholine, no longer counterbalanced by adequate dopamine, becomes the dominant influence, pulling movement toward stiffness and rigidity rather than smooth, fluid motion.
Cognitive changes also play a role. As cognitive abilities decline, safety awareness and reaction speed decrease, which can make people more hesitant and less confident moving through the world.
Shuffling and freezing affect some people with PD and involve more than just reduced movement size. There is a cognitive component: the ability to adapt and react in real time is also compromised, which contributes to getting stuck or losing a normal stepping rhythm. Anxiety compounds this, causing freezing and shuffling to occur in predictable places.
Dual-tasking, the ability to do two things at once, is also closely tied to walking ability. Alternating between a cognitive task and a physical task is something patients practice regularly, because it mirrors real-world demands and has a direct impact on how well people walk. Dopamine loss and cognitive changes together cause people to move smaller than they think they can.
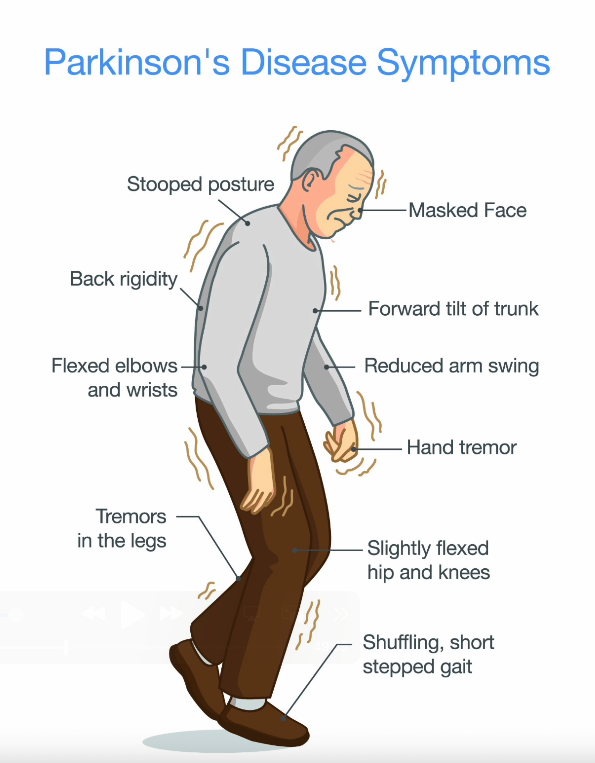
Three Gait Patterns
Bradykinetic Gait
Bradykinesia means small, slow movement, and it is one of the most common symptoms of PD. In walking, it shows up as slumped posture, a narrow base of support, and shortened step length, without an arm swing. Walking this way is exhausting: without a full step and without arm swing to build momentum, it takes enormous energy to cover any distance. People tire faster, go out less, and gradually do less overall, even if reasonably stable.
The narrow base of support also increases fall risk. Feet that stay close together make it harder to catch a stumble, and tripping over small obstacles becomes more likely. In the clinic, keeping feet wide is emphasized at every stage, whether standing, transferring, walking, or turning.
The main focus for treating bradykinetic gait is amplitude, meaning big movements. The brain in PD tends to underestimate how much effort movement actually requires, so the goal is to give people cues and targets that push them to move larger than they think they need to.
One of the most effective cues is heel strike: thinking about hitting the heel first with every stride. To do that, the foot has to reach out far enough to land heel-first rather than on the forefoot or midfoot. This increases stride length and walking speed right away. The recommendation is to practice it in intervals throughout a walk, setting an alarm every four or five minutes and focusing on heel strike for one minute before returning to a normal pace.
Arm swing works the same way. At a fast enough pace, arms swing naturally to counterbalance the legs. Cueing heel strike often brings the arms along. A useful real-world check is to look straight ahead while walking and see whether both arms are visible swinging in peripheral vision on each side. If only one arm is visible, more effort is needed on the other side. If neither arm is visible, both need attention. This is an easy way to carry amplitude training into everyday walking without any equipment.
In the clinic, forced-use training, which means making the body work harder than it would on its own, builds on the same principle. People walk on treadmills at increased speeds, sometimes with resistance bands around the waist to simulate walking uphill. The added resistance requires more effort and helps ignite the brain’s movement output.
Visual cues on the floor, agility ladders, small hurdles, dots, or painters tape also help people retrain bigger steps by giving the brain a distinct target to step to or over.
Step tracking with an Apple Watch or Fitbit adds another layer. If someone walks the same loop every week, the goal is to complete it in fewer steps over time, which means each step is getting longer. Reducing step count by 10% on a familiar route is a concrete, measurable goal that keeps attention on taking bigger steps.
Shuffling Gait, Festination, and Freezing
Shuffling and festination, a pattern in which steps become rapid and uncontrolled, share some characteristics with bradykinetic gait but involve an additional cognitive component that makes them harder to address through movement alone. People may find it hard to take that first step and end up shuffling, especially in tight or narrow spaces.
Freezing of gait, where a person gets completely stuck and cannot take a step, can also occur and carries a higher fall risk. Freezing tends to happen in predictable places: transitions from carpet to tile, doorways, elevators, tight turns in bathrooms or kitchens. Initiation of movement is its own challenge, separate from sustaining walking once underway.
The underlying issue is weight shifting. Taking a full stride requires moving weight completely from one leg to the other. When that shift is incomplete, the body compensates by shuffling or jumping between legs rather than stepping cleanly. Building confidence with weight shifting starts in standing, not walking. Side-to-side weight shifts in a wide stance, practiced until comfortable, carry over into improved stepping.
Anxiety is a significant factor. The self-consciousness of shuffling, whether in public or in familiar spots at home, creates a negative feedback loop. Anxiety puts the nervous system on high alert, which in turn makes freezing and shuffling more likely. Breath control is a direct intervention: slow, deep exhalations when freezing feels imminent help downregulate that response.
Visuospatial impairment also contributes. People with PD can misperceive how far away a surface or wall is, making a normal-sized bathroom feel impossibly tight. The feet move smaller in response to a space that feels more confined than it actually is. In physical therapy, the work focuses on taking big, clean steps through those tight spaces, turning fully, and getting comfortable moving in the areas of the home where freezing and shuffling happen most.
At home, practical strategies include painters tape on the floor at problem spots to give a visual step target, self-cueing by counting steps out loud (“I’m going to get to the kitchen in 14 steps”), and a reset when freezing begins. A reset is: stop, take a deep breath and exhale slowly, shift weight back onto the heels, then feel the weight move side to side and go. A metronome, whether a physical device or an app, can also provide a rhythmic auditory cue to help keep stepping consistent and reduce shuffling.
A TheraBand stretched horizontally across the front opening of a walker frame gives people a tactile and visual target: reaching out to touch the band with every stride cues a longer step.
Stiff-Armed (Suitcase) Gait
Stiff-armed gait looks like someone carrying two heavy suitcases: arms locked at the sides, no swing, and very little upper body movement. It is caused by reduced trunk rotation. Normally, the arms swing during walking because the upper body rotates against the stepping leg, which counterbalances the legs and reduces the effort needed to move forward. Without that rotation, walking takes significantly more energy and people fatigue much faster.
Rigidity from the dopamine-acetylcholine imbalance is the root cause. PD symptoms often appear on one side of the body first, so one arm may stay locked while the other swings normally. Over time, both sides can be affected. Whether one side or both, the impact on balance, speed, and endurance is real.
Exercises that involve cross-body and rotational movement are the primary intervention. Yoga and boxing are both good fits because they involve constant, repetitive torso rotation. In the clinic, amplitude training for the upper body includes reaching side to side for targets, opening and closing the upper body in standing, sitting, and on all fours. The goal is to retrain the brain’s sense of how much movement is needed when walking.
Trekking poles are a practical tool for this pattern. They naturally extend the arms and promote reciprocal arm swing. Many people in the Pacific Northwest already use them for outdoor walking, and they are worth using consistently as a gait aid.
The peripheral vision check applies here too: both arms should be visible swinging while looking straight ahead. If one is not visible, pick up the effort on that side. If neither is visible, both need attention.
Assisted Devices
Finding the right assisted device requires trying options and evaluating what actually works for that individual. Choosing a device is not straightforward, and what a doctor recommends is not always what works best for a given person. Walkers, for example, can actually be less safe for people with shuffling or freezing gait because the walker can get away from them, or they may lose their balance reaching too far forward.
Trekking poles work well for some people and become a tripping hazard for others who hold them too high and forget to plant them. The U-Step walker has a built-in laser line, which is useful for freezing, but is extremely heavy, hard to get in and out of a car, and may not be practical for someone moving between multiple appointments in a day. It can be a good in-home option but often cannot travel with the person.
Medical supply stores often carry demonstration models of specialty walkers and other devices, which allows for a test run before purchasing. Seeing a physical therapist to evaluate options and try them in a controlled setting is the most reliable way to find the right fit.
Wearable Devices and Emerging Technology
Technology is moving into gait training in new ways. The same principle behind painters tape and agility ladders, giving the brain an external cue to step bigger, is now being built into footwear.
Neue Shoe is a smart shoe with technology embedded in the sole. It connects via Bluetooth to a phone and vibrates each time the heel lifts off the ground, continuing to vibrate until the heel comes back down. The goal is to keep the vibration going as long as possible, which means taking a longer step. It is designed as a training device, and the Parkinson’s Fitness Project clinic has been using them.
Another company, Movive, is developing similar footwear technology. Smart socks are also available that track gait data, measuring how much time a person spends in each phase of the stepping cycle and providing feedback on where to improve.
Robotic devices worn around the hips and legs assist with reciprocal limb movement and have been used in spinal cord injury rehabilitation for years. Research in PD is ongoing, and these devices are expected to become more widely available.
Laser pointer canes and laser attachments on walkers, including the U-Step, give a visual line on the ground to step to, which can help people with freezing initiate and sustain movement. Some people simply carry a laser pointer in their pocket for the same purpose.
Audience Q&A
Q: What are your thoughts about a postural corrector to improve scapular retraction?
A: Postural correctors range from braces that physically pull the shoulders back to Bluetooth-enabled electrode devices that buzz when posture drops past a certain angle. Both can be effective right away. The vibration cue gets attention and prompts correction in the moment.
The problem is sustained attention. Used all day, any postural corrector eventually becomes white noise. People stop noticing the cue and the correction stops happening. The better approach is to use a postural corrector in short intervals throughout the day, then try to maintain the posture independently for a period before using it again. Relying on it continuously means the brain never has to do the work on its own, and the correction will fade.